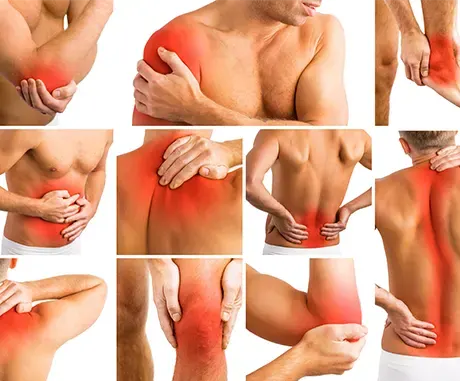
Guide pain · Acute and chronic
Pain is a very complex phenomenon with totally different qualities, intensity and characteristics. Acute pain is defined as short-term and locally defined. Longer lasting states of pain and chronic pain incl. chronic pain syndromes can also become independent disease patterns.
There is no uniform definition of chronic pain yet. Pain is a subjective sensation that every being perceives in a different way. It does not necessarily need to have a physical cause. Between 10 and 12 million people in Germany suffer from chronic pain.
Pain reduces the quality of life
What can be done in cases of acute or chronic pain?
What is pain?
The International Association for the Study of Pain (IASP) defines pain not only as the sensation of a damage of tissues but also as an experience of an unpleasant sensation or feeling. Pain is induced by a series of complex processes controlled by the nervous system. It occurs when pain receptors are stimulated which then send those signals through the spinal cord to the brain. The pain receptors (nociceptors) react to potential or actual injuries of tissue.
The quality of pain describes its severity and is a sensory perception. Pain can be perceived as dull, burning, sharp, piercing or tearing. As the psyche also plays an important part in the sensation of pain, it is also characterised by the emotional feeling connected with it, i. e. as torturing, killing or exhausting. It is important to note that the brain’s assessment of stimuli activates the experience of pain. The sensation of pain is therefore different from a direct pain stimulus that is medically defined as nociception. Nociceptors are activated as soon as a certain level is exceeded. They warn us of injuries to tissues for example.
Kinds or modes of stimuli are differentiated into:
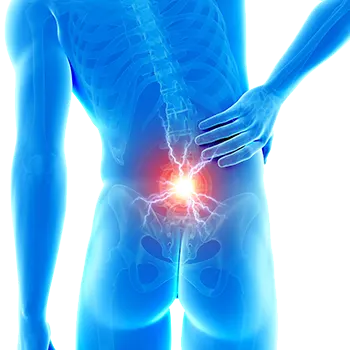
Where does pain come from?
The perception of pain is a characteristic of animalistic organisms that is essential for survival. Without the perception of pain, there is no warning system so that the body can easily be damaged and disease and even death are risked. About 80 percent of all nerve fibres outside of the brain and the spinal cord belong to the pain perception system. On general, pain receptors are present in nearly all tissues in the body. Only the brain and the liver tissue (liver parenchyma) have none.
The reception of pain happens in the nociceptors, the specialised nerve fibres that are situated in the whole body. They send their signals through the spinal cord into the brain where the excipation is processed and interpreted as pain. The sensors of the nociceptors are directed at mechanical and thermical stimuli as well as chemical substances (e. g. neurotransmitters) which are released in case of injuries or infections of the tissue. The stimuli or substances increase the sensitivity of the nociceptors and release nerve impulses.
Nociceptive and sensorimotoric signals are interconnected in the spinal cord. How fast a stimulus reaches the spinal cord depends on the type of fibre. There are fibres that transmit the primary pain signal into the spinal cord or activate reflexes, which is then perceived as sharp. Transmission by other fibres is more slowly and triggers dull and piercing pain. Pain perception describes the conscious perception of quality, localization, severity, duration and frequency of pain.
Types of pain receptors:

Commen causes for pain · What triggers pain?
Following modest estimations, in Germany alone approx. 10 million people suffer from constant pain that requires treatment. This includes all kinds of pain, that persist for longer than expected i. e. after surgery or in the course of an illness. They are described as chronic pain.
Pain and pain syndromes can appear in different ways. The most common kinds of pain are pain in the head, back pain, tooth pain, joint pain (rheumatism, osteoarthritis), pain in throat and ears, tumourpain, period pain, nerve pain and neuropathic pain (the so called phantom limb pain).
Pain caused by osteoarthritis, osteoporosis, fractures, rheumatism, tumours and diabetes mellitus are very frequent in old age. The presence of medium to severe pains are risk factors for the development of chronic postsurgical pain (Perkins und Kehlet, 2000; Bisgaard et al., 2005; Nikolajsen et al., 2006).
Back pain
Back pain is very widespread and one of the most common reasons for consulting a doctor. They are also one of the main causes of inability to work in Germany. Nearly every third adult person suffers from frequent or permanent back complaints. As a rough guide: If strong pain persists for three days, a medical consultation should be done to determine the cause.
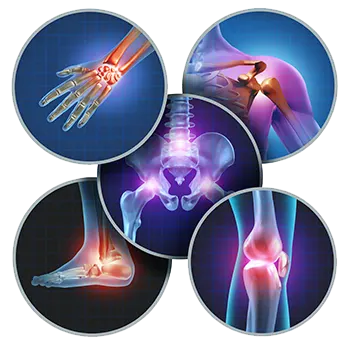
Joint pain
Joint wear or osteoarthritis is by far the major joint disease that causes joint pain. It can appear on different joints like hand, finger, foot, knee or shoulder. Acute joint inflammations (rheumatoid arthritis, gout, bursitis or borreliosis) as well as injuries like sprains, wrenches, torn ligaments or pathological weight bearing are also common causes for joint pain. Complaints with joints and muscles are often a consequence of previous, not fully healed sports injuries or long-term pathological stress in job and every day life. Joints, muscles, ligaments, tendons, bones and nerves that have been damaged like this and the resulting pain can be a severe impairment of the quality of life. Pain is also a main symptom of degenerative diseases of the musculoskeletal system. Osteoarthritis usually causes patients to suffer intense pain when bone rubs against bone due to the loss of cartilage in the joints. Frequent fractures, especially of the vertebral bodies, are a source of pain for osteoporosis patients.
Joint pain is categorised in:
Postsurgical pain
Postsurgical pain is caused mainly by the incisions into the skin and the relocation of parts of the tissue, bones and fragments of bones for example, which has a massive impact on the surrounding tissue and can lead to postsurgical pain. Intensity and duration of postsurgical pain vary a lot and they can affect bodily functions in several ways. Postsurgical pain is not only very unpleasant for the patient but can also have a negative influence by impeding normal wound healing processes. The normal pain reaction following surgery helps to prevent premature weight-bearing. But if the pain is too severe it can lead to a stress reaction and also impair mobilisation and breathing which causes complications (i. e. pneumonia). About one quarter of the patients suffers from severe pain on the first day postsurgical, nearly half from moderate to severe pain. It is remarkable that not only extensive surgery can lead to severe postsurgical pain but also by comparatively small interventions.
Wound pain resp. pain due to wound healing
Most important on general is how the patient experiences the pain. All kinds of pain in connection with wounds and also pain that develops in the healing process is called wound pain. In the areas concerned, the body produces substances that trigger pain depending on kind and severeness of an injury. Chronic wounds are usually acommpanied by a more or less severe wound pain. A partial or complete disorder of the experience of pain can be caused by diabetic PNP (polyneuropathy) which may result in delayed diagnosis of inflammations. Medical experts need to know very well which product has to be used in the respective phase of wound healing.
Classification · Grades
For millions of people, pain is a constant companion. Many of them live in fear of a renewed attack, sometimes getting into a vicious circle of pain and fear.
Acute pain
Acute pain can be essential for survival. Usually its cause can be clearly defined. The consequential physical reactions have the task of supporting rest of injured or affected organs and body parts which helps to prevent further damage.
Chronic pain
Chronic pain does not only massively reduce the quality of life of those affected, it can also have multiple consequences. Inability to work up to early retirement for example can have a negative influence on the patient’s living conditions. A very large number of sick leave days also has an economic relevance.
Pain memory
Persisting pain can become an independent pathology. Nerve cells, spinal cord and brain become increasingly more receptive for pain stimuli. Even light stimuli can then trigger a sensation of pain. The experience of pain can also be influenced by the individual behaviour and emotional and psychic factors. If these various factors mutually influence each other, a vicious circle, a spiral of pain can develop. Pain stimuli can trigger synaptic and cellular changes in the spinal cord that are similar to the processes of memory building. A "pain memory" develops. The signals of the nociceptive system become interconnected and are processed together which can intensify them so that the organism reacts with a chronification of the pain.
Consequences of chronic pain
If treatment of pain does not begin on time, that can result in a reaction of the nervous system including the danger of chronification. This is often described as memory of pain (or pain engram). Originally, the reaction was triggered by acute stimuli but it persists even when the causes for the pain have receded or vanished. A typical symptom is that formerly seldomly occurring pains become more frequent and persist for an increasing amount of time. In the course of this advancing chronification even complaints in other parts of the body may be triggered. Many chronic pain patients suffer from listlessness and a lack of motivation. They are desperate and lost all hope, suffer from anxiety or depression and a reduced self-esteem. If outpatient treatment is not sufficiently effective in this case, an inpatient treatment in a specialised pain clinic may be necessary.
Treatment options
The WHO schematics of pain describes a three-layered plan for pain treatment that many practitioners adhere to. It is largely medicinal:
Basic diagnostics
A thorough anamnesis by a doctor in an MBST treatment centre is the start of a conclusive basic diagnostics. The patient should describe his complaints as detailed as possible, for example when and where the pain started, since when it is present including potential triggers. The intensity and quality of the pain, dull, piercing or tearing, should be mentioned. To collect information about previous or chronic diseases as well as family history, the past situation is discussed in the consultation. At last, the patient’s living conditions and mental state of health with possible depressions or stress situations are included in diagnostics.
MBST in the treatment of acute and chronic pain
Molecular biophysical stimulation
MBST therapy is based on the physical principle of magnetic resonance, in which hydrogen nuclei take up energy and then release it again partly into the surrounding tissue. Scientific data suggests that MBST magnetic resonance technology stimulates various biophysical processes and triggers anti-inflammatory and pain-relieving effects.[1,2,3]
A highly significant reduction of the subjectively experienced intensity of pain as well as a sharp decline of pain frequency in various clinical pictures was apparent in studies.[4,5,6] These effects could often be verified years after the treatment. The number of sick leave days of employed patients due to back pain was reduced considerably.[7]
The advantages of MBST magnetic resonance therapy in cases of osteoarthritis at a glance:
[1] Temiz Artmann et al. 2011, Methods and Findings in Experimental and Clinical Pharmacology, 27(6), 391–394 · [2] Melzer et al. 2003, Fachkrankenhaus für Orthopädie · [3] Steinecker-Frohnwieser et al. 2014, J Orthopedics Rheumatology, 9/2014 · [4] Kullich et al. 2013, SCHMERZ nachrichten 4a · [5] van Laack et al. 2011, Orthopädische Praxis 47, 11/2011, 536–543 · [6] Steinecker-Frohnwieser et al. 2009, Bone 44, 295, doi: 10.1016/j.bone.2009.03.537 · [7] Salomonowitz et al. 2011, Z f. Orthopädie und Unfallchirurgie, 149, 575–581 · [8] Kullich/Melzer 2018, Scientific evaluation of the MBST Magnetic Resonance Technology regarding the therapeutic potential and proof of clinical efficacy


MBST-Arthrosetherapie · Kurzer Überblick